Psoriasis: When the Immune System Affects Skin
An overview of psoriasis: what it is, why it happens, how it’s recognized, and ways you can manage daily life with understanding and care.
Understanding Psoriasis: What You Should Know
Psoriasis is a long-lasting condition where your immune system causes skin cells to grow too quickly. This leads to patches of inflamed skin with a layer of scaly, dead skin on top. It is classified as an immune-mediated skin disease (sometimes referred to as autoimmune) and is not contagious. Psoriasis tends to go through cycles, flaring for a few weeks or months and then subsiding for a while.
Anyone can develop psoriasis, no matter your age or background. It often begins in adulthood and affects men and women equally. In the United States, it’s estimated that over 3% of the population (around 7.5 million people) lives with psoriasis. This condition is discussed widely today because it can impact daily comfort and confidence. Knowing the basics about psoriasis can help you understand what it is and support those who experience it.
Why It Develops and How It Appears
Researchers believe psoriasis develops from a mix of genetic and immune factors. Certain immune cells attack the skin by mistake, leading to rapid skin cell growth. If you have family members with psoriasis, you may be more prone to it. Triggers like infections (for example, strep throat), stress, skin injuries, or some medications can contribute to flare-ups. It’s important to remember psoriasis isn’t caused by anything you did (and it’s not due to poor hygiene). The exact cause isn’t fully understood.
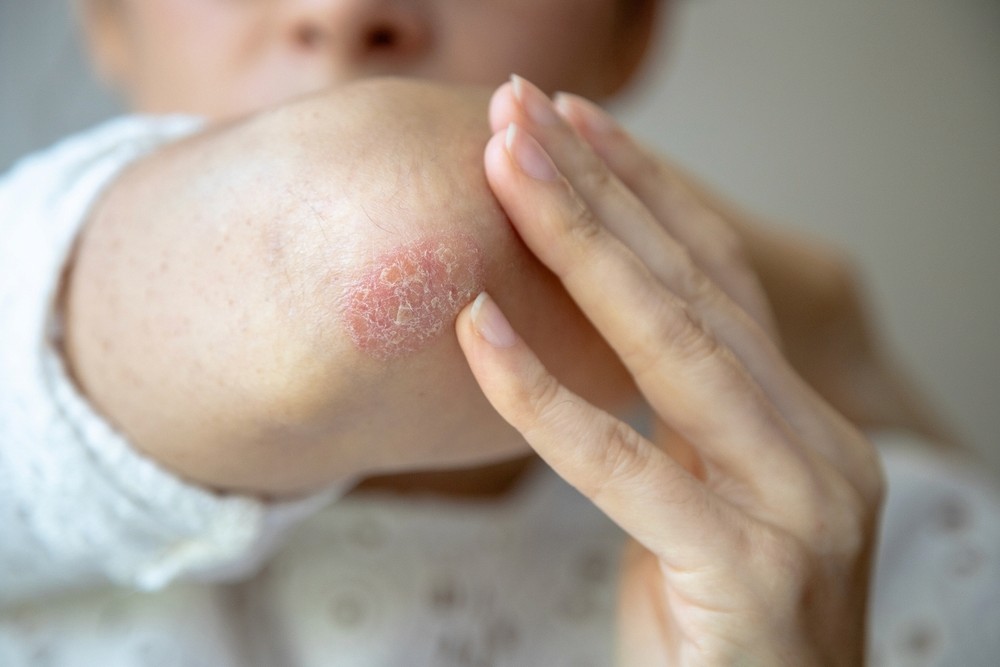
Psoriasis often appears as red, raised patches of skin covered with silvery-white scales. These patches (called “plaques”) can itch, burn, or feel sore. You might notice them on your elbows, knees, scalp, lower back, or other areas of the body. The patches can become very dry and may crack or bleed if irritated. Sometimes psoriasis also affects your fingernails or toenails, causing pitting (small dents) or changes in color. Every case can look a bit different, and symptoms often come and go over time.
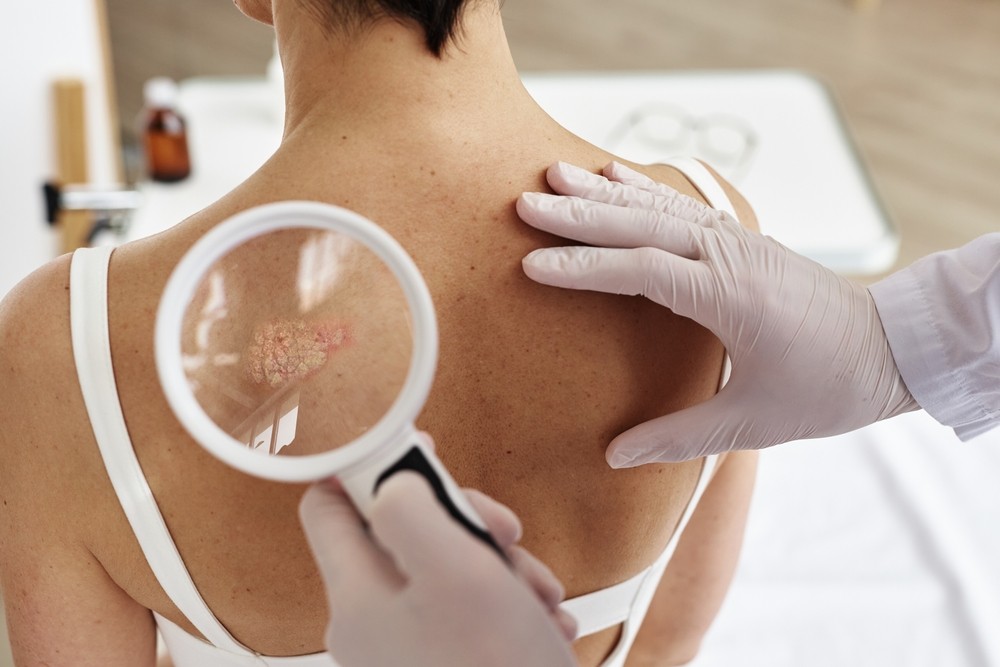
How It Is Commonly Identified
Psoriasis is usually identified by its distinct appearance. You might first notice something is off when you see persistent scaly patches or feel itching that doesn’t go away. Because psoriasis plaques have a unique look (red or discolored skin with silvery-white scales), a doctor can often recognize it with just a skin exam. There is no specific lab test for psoriasis – the rash’s appearance is the main clue.
If you visit a healthcare provider about your skin, they can confirm psoriasis by examining it and asking about your history. In some cases, a small skin biopsy might be done to rule out other issues. Identifying psoriasis early on gives you the chance to learn your triggers and start caring for your skin to ease discomfort sooner. Early recognition isn’t about a cure (there is no cure), but about understanding what’s happening so you can manage it day by day.
Different Forms and Stages You May Hear About
Plaque Psoriasis
This is the most common form. If you have plaque psoriasis, you may notice dry, raised red patches of skin (plaques) covered with silvery-white scales. These plaques often appear on your elbows, knees, scalp, or lower back. They can be itchy or tender, and the skin around them might feel tight or sore.
Guttate Psoriasis
A form that often affects children or young adults, sometimes following a strep throat infection. It appears as many small, drop-shaped spots across your trunk, arms, or legs. Guttate lesions are usually finer and thinner than plaque lesions. This type may come on suddenly in a single outbreak.
Inverse Psoriasis
This type shows up in body folds and creases. You might find smooth, red patches of irritated skin in areas like your armpits, under the breasts, or around the groin and buttocks. Inverse psoriasis doesn’t have the thick scales; instead, the patches are shiny and inflamed, and they can get worse with sweating or friction.
Managing Daily Life With Psoriasis
Living with psoriasis means finding ways to stay comfortable while taking care of your skin and overall well-being. One important habit is to keep your skin moisturized regularly. Using a gentle moisturizer every day (especially after a warm bath or shower) helps prevent dryness and cracking. Stick to warm or lukewarm water instead of hot when you bathe, since hot water can dry out your skin and aggravate inflammation. Use mild, fragrance-free soaps or cleansers to avoid irritating your skin. It may help to gently pat yourself dry with a soft towel and apply a moisturizing cream or ointment right away to lock in moisture. Many people also find it useful to use a humidifier at home to add moisture to the air during dry weather.
Pay attention to your daily routine and try to identify any personal triggers that make your psoriasis worse. For example, if stress tends to bring on flare-ups, finding ways to manage stress (like meditation, deep breathing, or a calming hobby) can sometimes support your skin’s calmness. Getting enough rest and maintaining a balanced diet can benefit your body too. While food isn’t a proven cure, some individuals notice improvements when they eat plenty of fruits, vegetables, and whole grains. Avoiding heavy alcohol use and not smoking can also be beneficial for your skin and overall health. Most importantly, give yourself grace and flexibility. Psoriasis can have good days and bad days, so listening to your body and doing what feels comfortable (like wearing soft, breathable clothing to reduce irritation) can make a positive difference.

Simple Precautions That Can Support Safety and Comfort
Be gentle with your skin. Try to avoid cuts, scrapes, and sunburn, since even minor skin injuries can trigger new psoriasis patches. Use sunscreen and protective clothing in the sun, and wear gloves for activities like gardening to shield your skin. Also, keep your nails short to reduce accidental scratching and lower the chance of infection.
Wear loose, soft clothes (like cotton) so you don’t irritate sensitive skin. Keep your home comfortable (not too hot or too dry). For example, using a humidifier in winter can help keep your skin from drying out. If you feel itchy, try a cool compress or a gentle moisturizer instead of scratching. It also helps to test new skin products on a small area first to make sure they don’t cause a reaction. Everyone’s psoriasis is a bit different, so adjust these tips to what works best for you.
Myths vs. Facts: What You Should Know
Myth
Psoriasis is contagious
Fact
It is not contagious at all, you cannot catch psoriasis from someone else.
Myth
Psoriasis is caused by poor hygiene
Fact
It has nothing to do with cleanliness. Psoriasis is driven by immune and genetic factors, not by being dirty.
Myth
Nothing can be done for psoriasis
Fact
There is no cure, but many people manage their symptoms and find relief through various care strategies.
Myth
Psoriasis is rare
Fact
Psoriasis is fairly common, affecting around 7.5 million people in the U.S.
Why Awareness Still Matters
Understanding psoriasis is important. Even today, many misconceptions persist, which can lead to stigma. In the United States, stigmatizing views of psoriasis are still common, but public education can reduce these negative attitudes. By being aware, you can replace myths with compassion. If you or someone you care about has psoriasis, you’re better prepared to offer support and encourage early management. For millions of American families, greater awareness fosters empathy, reduces isolation, and reminds those affected that they are not alone.
Common Questions You May Have
Is psoriasis contagious?
No. Psoriasis is not contagious. You cannot catch it from another person’s touch or by sharing personal items. It develops from factors inside your body, not from an infection.
Does psoriasis ever go away completely?
What triggers a psoriasis flare-up?
Are there ways to care for psoriasis day-to-day?
Trending Articles
Helpful reads on diseases, therapies, and daily health choices.
my
health
wisdom
Simple information for everyday health decisions.
© 2026 MyHealthWisdom. All rights reserved.
The information on this website is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have. Never disregard professional medical advice or delay in seeking it because of information you may have read on this website.

